Thinking in the worst case scenario is safe, but the opposite can be true
Objective
In this clinical situation we want to enhance the importance of a proper differential diagnosis in the attention of a patient, including all the possibilities that can explain the symptoms of the patient.
Clinical Case
A 62-year-old woman had a diagnosis of a kidney cancer with bone metastases. She was receiving treatment for her disease in the last year, but, after some general improvement, she had to stay at the hospital due to an impossibility for walking, with a strong pain in her back irradiated to both legs, more intense in her left leg.
The doctor in charge of the patient wanted to rule out the presence of a spinal cord compression. She asked for an MR of the dorsal and lumbar spine because her level of suspicion was very high, after the patient referred a strong pain in her back, a loss of strength to move her legs, and a doubtful sensitive level corresponding to the T12 metamer.
Clinical Evolution
The pain improved after a treatment with oral morphine, but the patient was nor able to walk properly. The report of the MR showed the presence of spinal metastases, but without a cord compression. Then, the physician decided to ask for a plain radiograph of the femur and the hip, and the image is shown here:
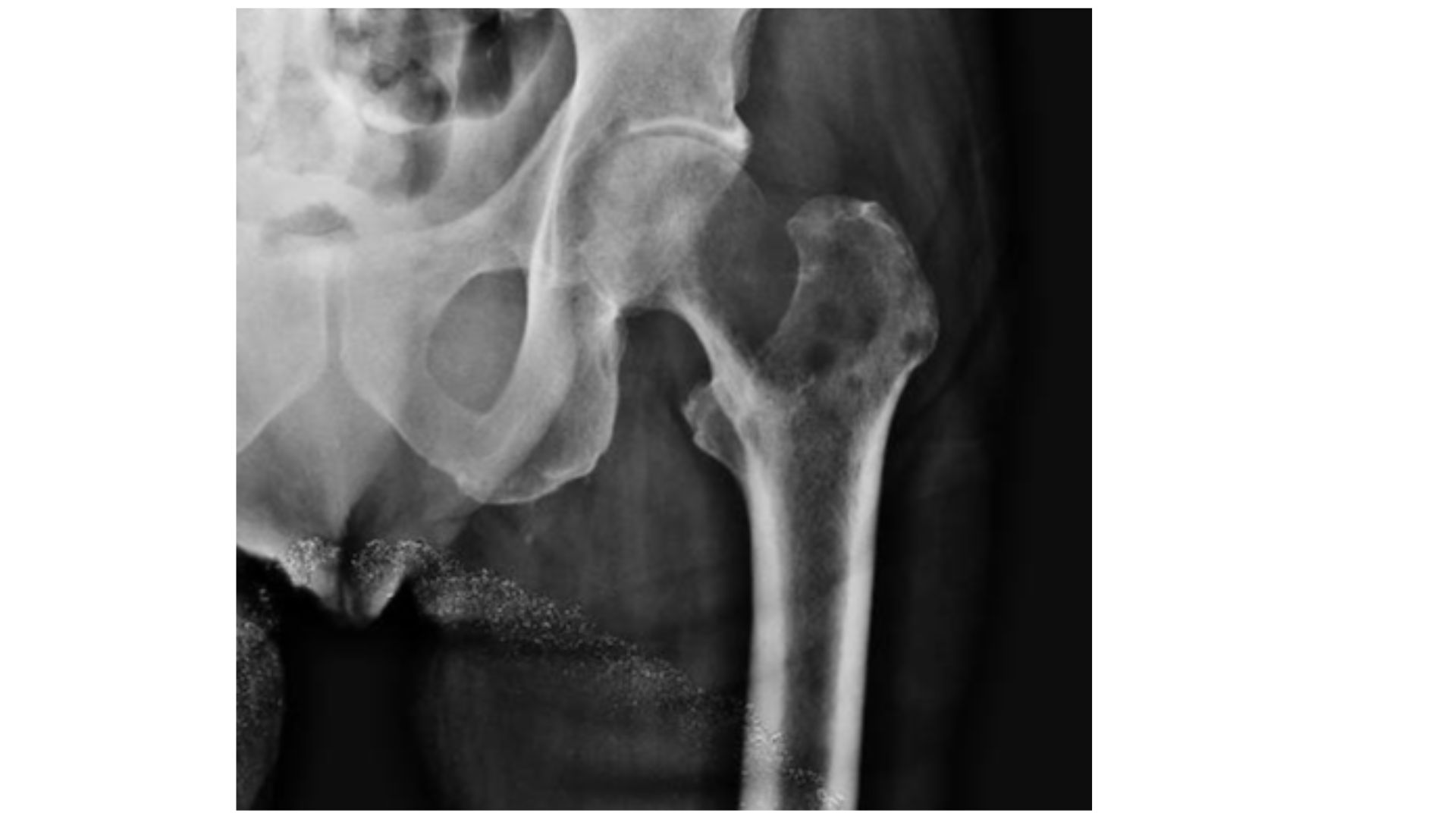
Final Comment
The strategy of thinking in a “worst-case scenario” is useful to discard urgent and serious clinical problems. This way of reasoning in clinical practice is a way to include in the differential diagnosis some diseases that can be life threatening to the patient, but this strategy must be accompanied with a complete checking of the anatomy and physiopathology.
Author: Dr. Lorenzo Alonso Carrión
FORO OSLER




