Pseudothrombocytopenia: a system analysis for a good detective
Pseudothrombocytopenia : a system analysis for a good detective
Clinical case
A 59-year-old woman was receiving treatment with radiotherapy and weekly cisplatin, after a diagnosis of cervical cancer. After three weeks her platelet level was under 20.000 and she was put under
observation. There were no signs of splenomegaly or liver disease. She was treated with prednisone but she maintained a low platelet count reported by automated hematology analyzers.
Clinical evolution
The patient was not receiving prophylactic heparin due to the low platelet count, an she was asymptomatic. The platelet count reached a peak value of 60.000 when a “manual” count was made by a technician. After a week in the same situation a peripheral blood smear showed platelet clumping, an explanation for the low platelet count (pseudothrombocytopenia). The term pseudothrombocytopenia is used to define a state with a falsely low platelet count reported by automated hematology analyzers due to platelet clumping.
Final Diagnosis: Pseudothrombocytopenia. Commonly, this clumping is caused by an alteration of the platelet surface glycoproteins when they are incubated with a calcium chelator such as EDTA. These modified platelet antigens, then react to anti-platelet autoantibodies. The machine can discriminate for individual platelet inside these clumping.
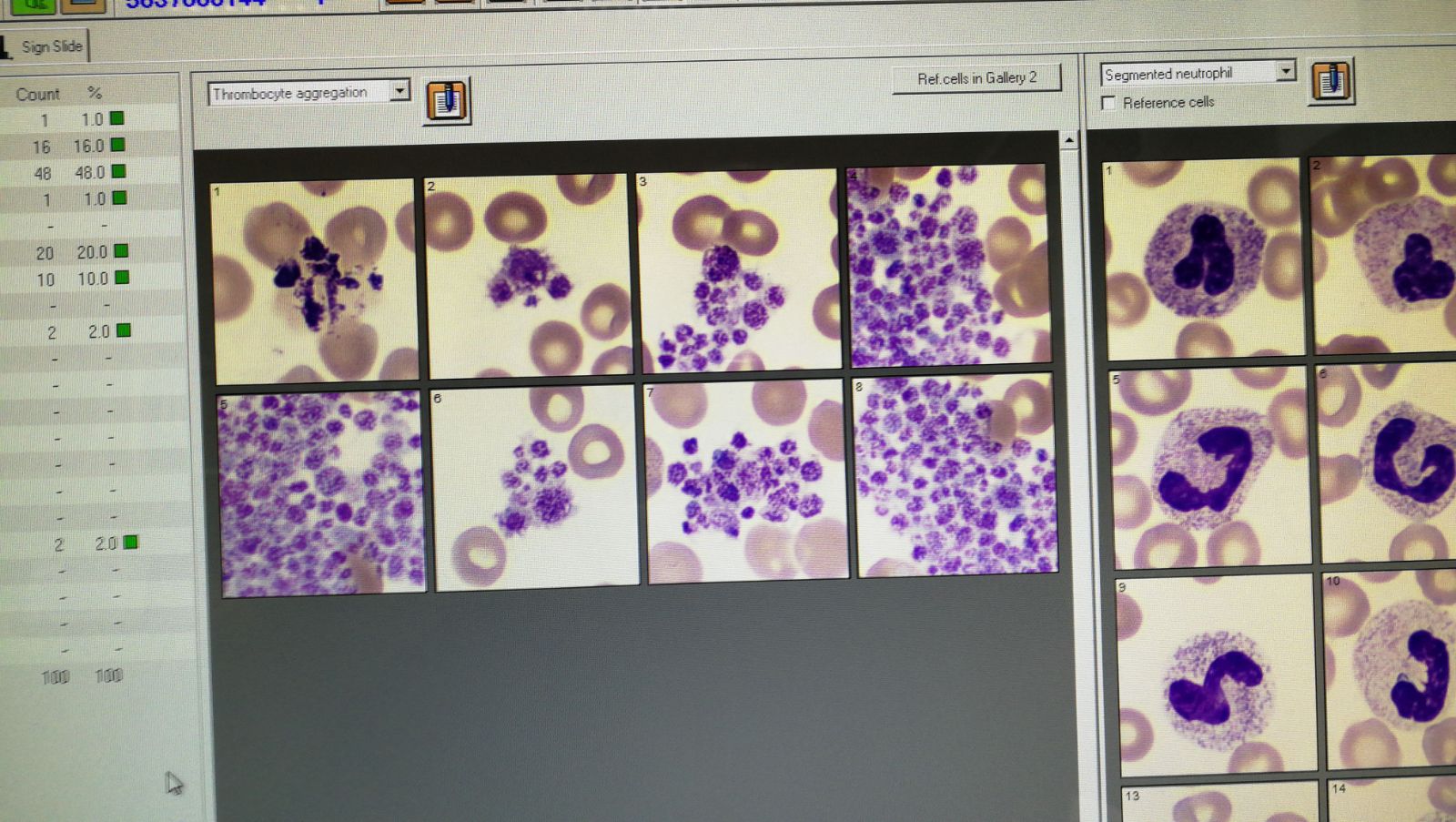
Platelet clumping
Comment
A simple clinical situation like this put the patient at risk for several reasons:
1) Pseudothrombocytopenia delayed the treatment for a curable disease, increasing anxiety in the patient.
2) The patient was not treated with prophylactic heparin, due to the misconception about the platelet count.
3) There was a bleeding risk with a high probability to indicate a platelet transfusion.
Analysis
This case shows the direct relationship between the “system” and the clinical reasoning process. We believe that an automated process is always exact and safe, but exceptions to the rule can be always present, as it was in the case when EDTA was used as an anticoagulant. When the concordance between clinical situation and data is not logical, our clinical judgment must always prevail. A system problem was at the base of a diagnostic error in this case.
Bibliography
Bizzaro, N., et al. (1995). EDTA-Dependent Pseudothrombocytopenia: A Clinical and Epidemiological Study of 112 Cases, With 10-Year Follow-Up. American Journal of Hematology, 50, 103-109
Van der Meer, W., Allebes, W., Simon, A., van Berkel, Y., & de Keijzer, M. H. (2002). Pseudothrombocytopenia: A Report of a New Method to Count Platelets in a Person With EDTA- and Temperature-Independent Antibodies of the IgM Type. European Journal of Haematology, 69, 243-247




