Clinical reasoning: Edema, Orthopnea
Objective
The main objective of this case is to show that representation is a strong bias, and the only possible antidote is to open the list of causes that could be involved in a clinical situation.
Clinical case
A-60-year-old man had a diagnosis of lung adenocarcinoma. He started a treatment under a clinical trial protocol, with a combination of chemotherapy and immunotherapy, with an experimental drug.
A week after his second treatment, scheduled every three weeks, he was admitted to the hospital with an acute shortness of breath, a non-productive cough and a fever around 38 degrees Celsius. He was not taking any calcium blocker agent.
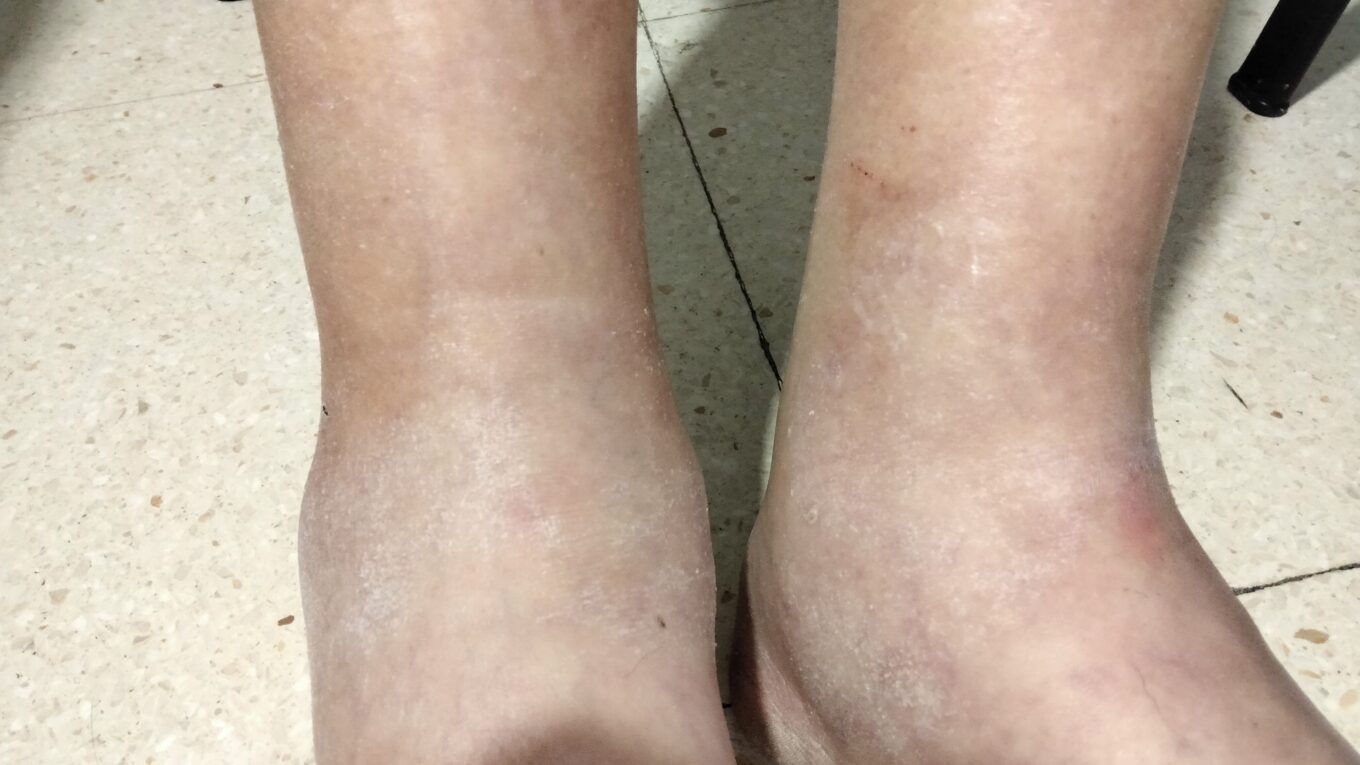
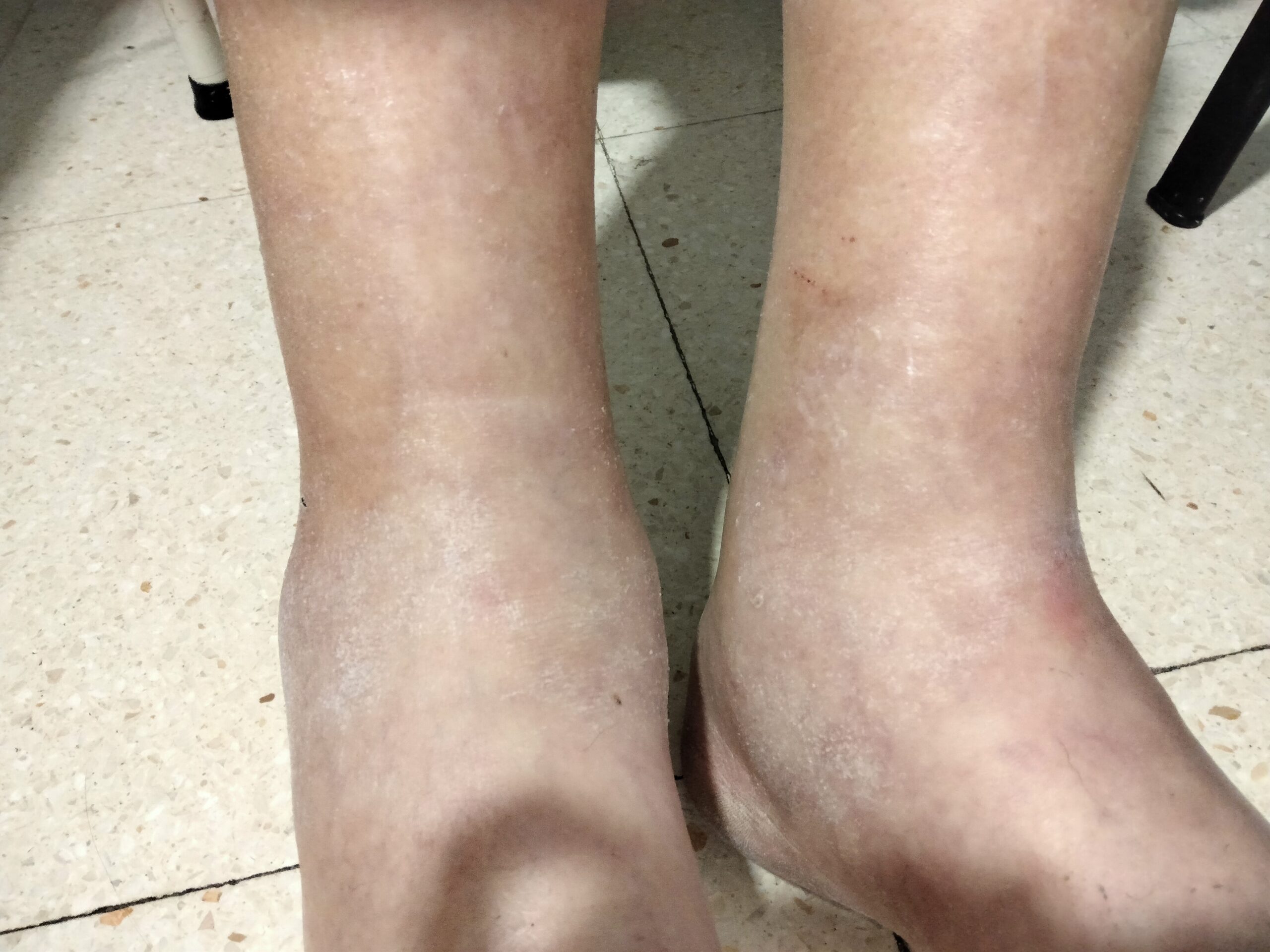
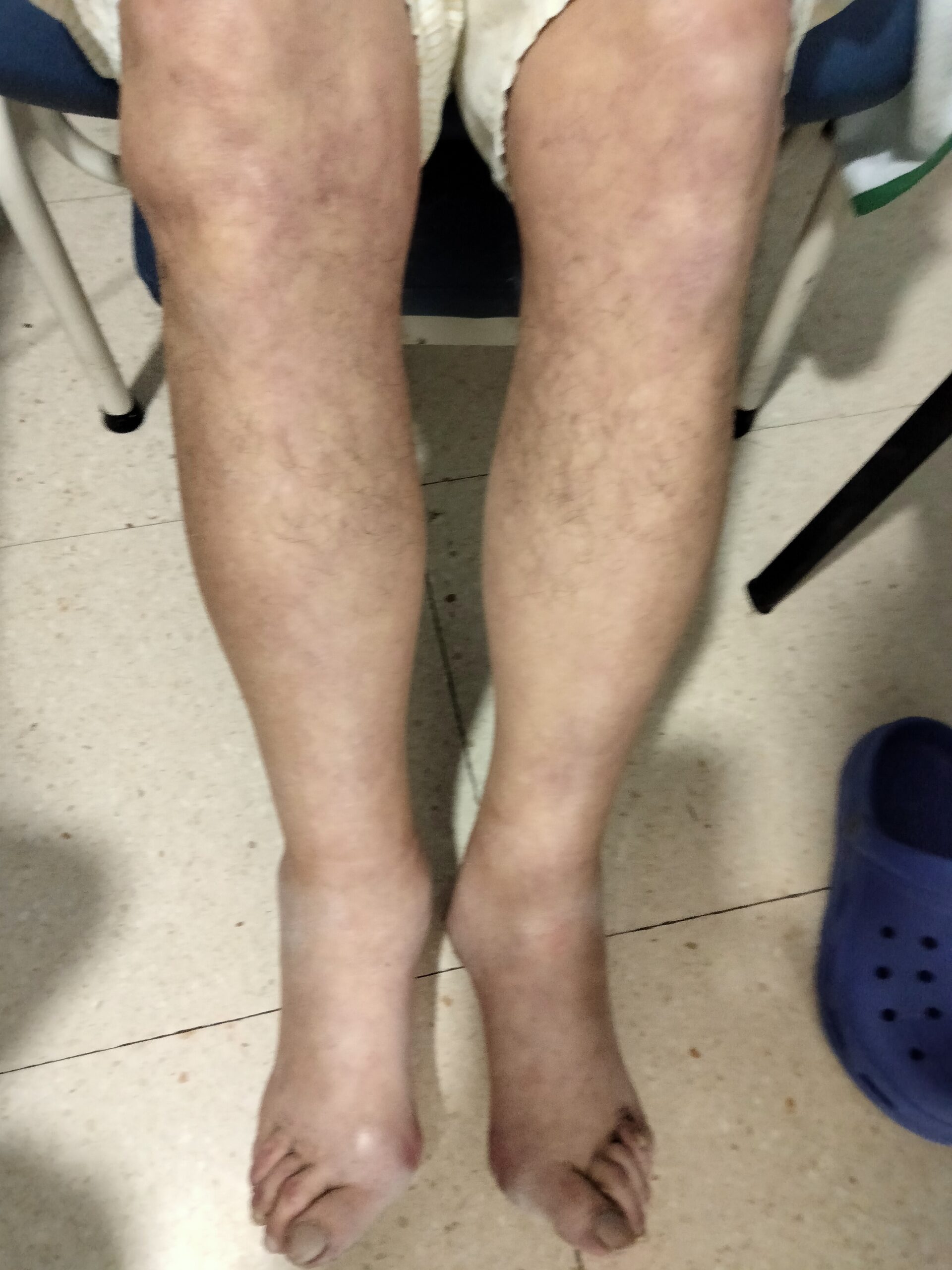
The physical examination showed a right pleural effussion and both ankles simmetrically swollen, and two days later the fluid retention reached both knees. No jugular venous distention was present. He had no hepatomegaly or splenomegaly. Both legs had a bilateral soft tissue edema, from the knees to the ankles, without pain or erythema.
Blood cultures were negative. No sputum could be obtained for a sample.

The X-ray showed an improvement in the lung tumor, but an increase in the right pleural effusion together with a mild pericardial effusion and the infiltrates in the upper lobes.

Patient Illness Script (Problem representation)
” This is a patient with a diagnosis of lung cancer,who started in an acute way with pleural and pericardial effusions, both legs swollen and orthopnea, after a chemotherapy and immunotherapy treatment. My first assumption, linking edema and orthopnea, is a cardiac origin of the problem, probably associated with the treatment, maybe cardiac toxicity”
Clinical evolution
The echocardiography showed no valvular or myocardial problem, with a mild diastolic constriction in relation with the pericardial effusion. The ECG was also normal. The patient started treatment with broad spectrum antibiotics, high-dose of steroids and a right pleural thoracocentesis, with a clear clinical improvement in a week in his clinical situation, without shortness of breath or orthopnea and improvement in the fluid retention.
Comment
In a patient with orthopnea and both legs swollen, the first diagnostic suggestion is a cardiac problem, because this image is a strong representation or shortcut that we have in our mind. But, when you know that the myocardial and valvular function are normal you start to think in several other possibilities. The presence of a mild pericardial effusion, together with the pleural effusion and the bilateral infiltrates, can make you think in a generalized edema with interstitial pulmonary location associated.
The patient started to improve after the thoracocentesis and the treatment with antibiotics and a high-dose of steroids. We received the information that one of the experimental drug was associated with the possibility of generalized edema.
The edema in the legs and the pleural effussion disapeared almost completely, but the infiltrates in both lobes lasted for several days without a complete resolution. No diuretics were prescribed.
The representation heuristic is a useful shortcut to decide in a clinical situation, but we always must to be open to other possibilities, mainly when the patient is under a new treatment with drugs with a specific toxicity.

Final Diagnosis
Lung Adenocarcinoma, with pleural and pericardial effusions, leg edema, and a bilateral infiltrate in the upper lobes, edema possibly associated with a drug.
Author: Dr. Lorenzo Alonso
FORO OSLER