So easy, so common, but undiagnosed
A 45-year-old patient had a diagnosis of malignant melanoma with two axillary lymph nodes with metastases. He was treated with adjuvant subcutaneous Interferon, but he started with an episode of acute abdominal pain. His oncologist was challenged….
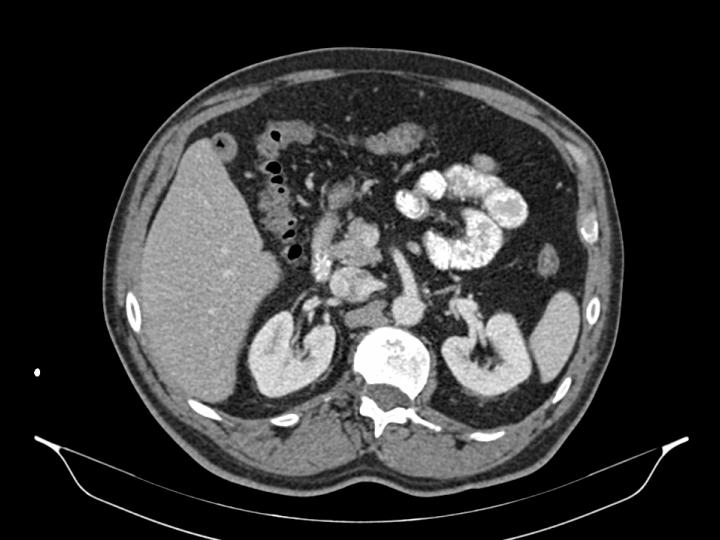
CLINICAL CASE: The patient has no previous important diseases. Abdominal pain started acutely, located around epigastrium and right hypocondrium, with nausea, vomiting and constipation. No fever or anemia was present. He was treated with fluids and analgesic with a complete resolution of the symptoms. His oncologist asked also for a colonoscopy that was informed as normal. A CAT scan showed here evidenced no major problems
CLINICAL EVOLUTION: A month later a second episode appeared and the patient was referred to the Emergency Department. After a new anamnesis and physical examination the doctor in charge makes a presumptive diagnosis of biliary colic related to the presence of gallbladder stones confirmed in a sonogram.
CLASSIFICATION OF THE PROBLEM: DIAGNOSTIC DELAY
ANALYSIS:
COGNITIVE ASPECTS: REPRESENTATION heuristics. The oncologist makes the assumption that the problem was related with melanoma, because this is one of the tumors with common disemination to the small bowell. This way of thinking changed the real prevalence of the problem. In the opposite situation a doctor working in the ED usually have this common pattern in mind, even for a male patient like this.
RADIOLOGICAL ASPECTS: The CAT scan was informed as normal in relation to the gallbladder. CAT scan is not the best test to explore the gallbladder, and cholesterol stones are even more difficult to see like in this case. The sonogram was more precise exploring the gallbladder.
SYSTEM ASPECTS: A lack of communication between the oncologist and radiologist.